
4 Considerations to Manage Your Total Cost of Medical Equipment Ownership
Want to lower your medical equipment total cost of ownership (TCO) while improving quality of care? These actionable strategies can help.
Solutions
Workplace Management Solutions
Real Estate Management Solutions
Maintenance Management Solutions
Energy Management Solutions
Engineering Document Management Solutions
Asset Management Solutions
Automate campus scheduling for classes, meetings, and exams with our EMS software.
Plan and manage conferences effortlessly with EMS software to impress guests and streamline operations.
Boost workplace flexibility and maximize space use with seamless desk and room booking.
Organize workplace or campus events smoothly, creating memorable experiences.
Optimize workspace, manage allocations efficiently, and reduce costs with our space management solutions.
Deliver projects on time and within budget by improving communication, collaboration, and efficiency with our software.
Streamline lease accounting for ASC 842, IFRS, and GASB compliance.
Manage leases efficiently by tracking key dates, analyzing costs, and ensuring compliance.
Centralize data and analytics for better insights, faster negotiations, and revenue growth.
Centralize facility and asset maintenance, automate work orders, and ensure compliance with our CMMS software.
Extend asset life, reduce downtime, and prevent costly repairs with data-driven monitoring.
Prevent equipment failures and extend asset life by detecting and addressing issues early.
Make sustainable, cost-efficient energy decisions by monitoring and optimizing power consumption.
Remotely monitor and control equipment with real-time data to predict issues, boost efficiency, and reduce downtime.
Easily share and collaborate on documents, creating a single source of truth for engineers and contractors.
Manage and analyze assets across their lifecycle to schedule maintenance, reduce downtime, and extend lifespan.
Improve visibility, automate work orders, and ensure compliance for efficient facility and asset management.
Resources
Browse our full library of resources all in one place, including webinars, whitepapers, podcast episodes, and more.
Self-Service & Support
Looking for self‑service training, best practices, helpful videos, product resources, or support? You’re in the right place.
About Accruent
Get the latest information on Accruent, our solutions, events, and the company at large.
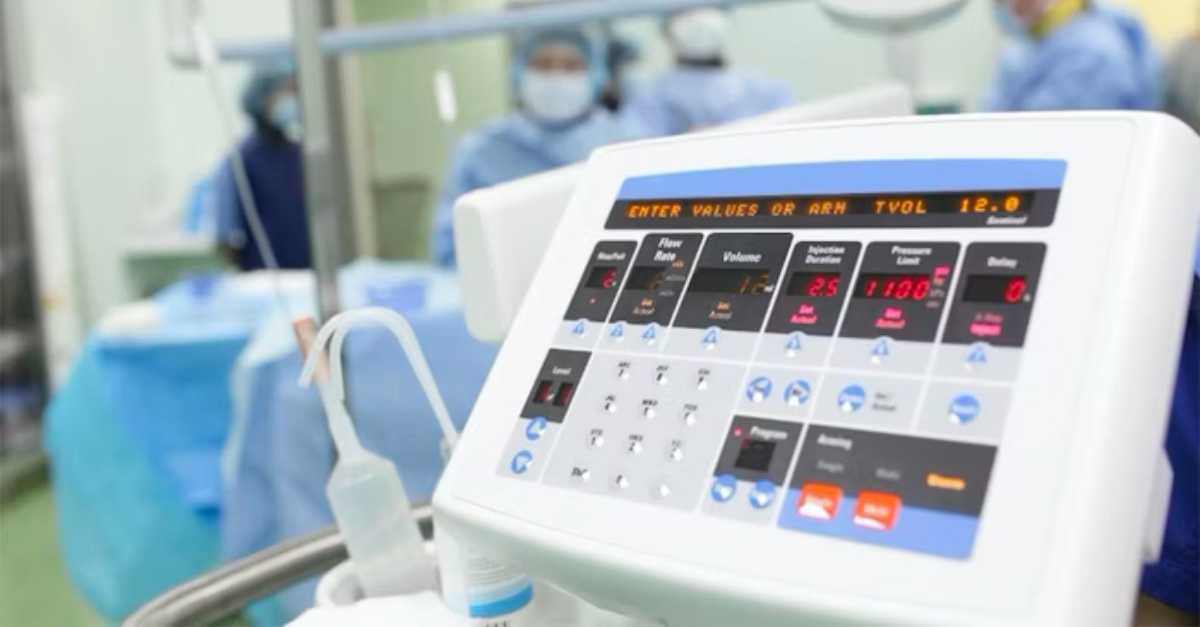
See how medical equipment data can be part of a broad strategic vision for managing investment in medical equipment.
By Eric Fischer, Data Insights Sr. Product Manager, Accruent
Early in my career, I had the privilege of meeting Earl Bakken, founder of Medtronic and inventor of the first wearable pacemaker. I was amazed to learn that a young Earl Bakken was inspired by the movie Frankenstein, which led him to believe that electricity could bring someone to life - something he proved to be possible. Through his inventions, he extended the lives of millions of people - including my father, who had a pacemaker implanted five years ago.
The lives touched by Earl's heroics and other brilliant engineers in the medical device industry is truly amazing. I see many headlines that claim that the US healthcare system is broken, but imagine what biomedical equipment alone has done to improve our health in the last few decades. Yes, there are stories of device failures, adverse events, kickbacks to doctors, and painful side effects and deaths due to some devices implanted during procedures. On the whole, however, medical devices have been a blessing to our world's health.
Consider the positive impact that ventilators have had on our response to COVID-19. Pandemic aside, how many lives have external automated defibrillators saved in emergency response situations. Imagine where we would be without infusion pumps, anesthesia machines, MRI machines, x-ray systems, echocardiograms, and patient monitors. Medical equipment is critical to modern healthcare today. In the future, medical equipment will be even more critical. Medical equipment is increasingly connected to hospital networks and data from devices can be integrated with electronic health records, tied to clinical outcomes, aggregated and analyzed to further improve patient health beyond what know is possible today.
Despite the criticality of medical equipment in promoting a healthy population, I am not convinced that hospitals understand the value of maintaining integrity and accessibility of their medical equipment data. My skepticism stems from the data I see flow in and out of Accruent’s asset management systems, used by 55% of U.S. hospitals to track and maintain medical equipment. Below are some of my observations and thoughts on how medical equipment data can be a part of a broader strategic vision for managing investment in medical equipment.
Over the past two years at Accruent, my job has been to aggregate and standardize medical equipment data from over 1,700 hospitals. In this work, I have noticed a few perennial problems associated with the integrity of medical equipment data:
The medical device industry is an extremely fragmented industry with a long history of mergers, acquisitions, divestitures, re-brandings, and resellers. As a result, the same medical device models may have twenty different legitimate names. Differences in how to refer to devices (ex. brand name vs. model number) are also part of the cause of this issue.
Finally, there are just differences in how hospitals enter data in free text fields (ex. misspellings). Even within a hospital system, it is common to have four or five different ways of referring to the same medical device in some cases. This makes it difficult to know how many of a specific model you have in inventory. Even to a well-informed medical professional, different ways of referring to the same device can confuse.
Standardizing categories is an art, not a science. The lowest levels of the popular GMDN and ECRI categories can be so granular that you can have almost as many categories as models. At a certain point, categorization is not valuable anymore.
Mapping these formal nomenclatures is also not a repeatable process with a useful MSA (measurement system analysis). I have seen the same medical device mapped to numerous different “standard” categories. A practical approach instead of a formal approach to categorization seems to be best with emphasis on being consistent within your categorization vs. mapping to a specific, formal nomenclature.
On average, 67% of a hospital's equipment recorded in a CMMS does not have a purchase price recorded. When it is entered, it is often not reliably inputted.
Many hospitals attempt to map devices to the American Hospital Association (AHA) regulations, which publishes standard useful lives for specific categories. However, mapping to AHA yields the same repeatability issues and inconsistencies as mapping to other standard nomenclatures. Furthermore, data is always changing, new records are added, and keeping pace using manual efforts is not sustainable. As a result, the data suggests that 49% of equipment does not have a recorded useful life.
Cleaning up the data does not sound like an intensive challenge, but it is. Priorities of keeping the equipment running, installing the new equipment coming in, and getting ahead of preventative maintenance always will overshadow the need for cleaning data. Budgets are tight so spending money to clean data rarely makes it to the top priority list. And it is not clear to healthcare executives how pursuing more reliable medical equipment data is foundational to managing medical equipment investments.
I have also noticed how little data is available on medical equipment in the public realm. The FDA and GUDID are obvious starting points, but I have found GUDID to be incomplete, and I have found that the FDA's searchability is antiquated. Most hospitals subscribe to paid services or their GPO to get data about medical devices when needed.
However, only a select few individuals in the organization tend to have awareness and access to the premium paid services that offer medical equipment information. Even then, this information is not always available on-demand and at the administrator's fingertips. In-house data is sometimes available, though this data is often hidden or buried in obscure back-office systems. Even if the in-house data was more accessible, I am skeptical about how clean and reliable it would be given what I have seen and mentioned earlier in this article.
There are also extended attributes of medical equipment that should be made published and accessible to decision-makers, such as the five listed below:
Documenting where a piece of fixed equipment is located and applying RFID tagging technology to track devices that are not stationary helps to track missing equipment and keep operations running smoothly.
Understanding who is financially responsible for equipment helps the capital planning process ensure that the appropriate stakeholders are held accountable in managing the equipment lifecycle.
Utilization can be helpful in many ways to understand when an item is due for replacement, if/when equipment is under or over-utilized, if the value is derived from a device, and if an institution needs an additional device to ensure capacity needs are met. Today, utilization data is often limited to modalities such as imaging.
Operating Systems are the underlying technology of an increasing number of medical devices, and they can have security vulnerabilities that hospitals should be aware of. This is especially true of outdated equipment, which are often built on less secure technology that is no longer patched and mitigated by the vendor.
Instructions for use are important for clinicians to understand how devices are intended to be used. Few healthcare institutions have all of these data attributes been bundled together in one spot and easily accessible to hospital administrators.
If all of this data were readily available and easily accessible by decision-makers, then it would pave the way for a better:
Easily accessible data will provide a smoother operation of clinical procedures, improved supply chain operations, and better financial outcomes.
Ultimately the reliability and availability of data can drive many other improvements in how investment in equipment is managed, including:
The Supply Chain group is an excellent example to start with. Haggling with vendors for a better price is not going to cut it anymore. To get to the next level of equipment cost reduction, Supply Chain needs to be more strategic, clinically integrated and savvy about how a hospital runs. To do this, they need to understand the lay of the land, and the best way to do that is with accessible medical equipment data and insights at their fingertips.
Supply Chain professionals need insights to tell them:
Supply Chain employees need to understand to what degree their institution adheres to standards versus giving in the Physician Preference Item requests, how much do new models in the market vary in cost, and most importantly, and how safe and reliable are these different models so that they can have meaningful dialogue with clinicians. Until Supply Chain is armed with this data, they will continue to struggle in the battle to reign in medical equipment costs.
Finance is another excellent example of a stakeholder who can improve their processes with reliable and accessible medical equipment data. Confidently knowing how much money is spent on medical equipment is key to managing expenditures. Forecasting expenditures can also become a pain point as coordination across hundreds of lead clinicians is a daunting and error-prone process.
Having a valid starting point could drastically cut the time spent on mundane capital planning processes while enabling a more efficient allocation of funds.
Clinicians, Patient Safety, and Value-Based Program Managers can also benefit from having access to medical equipment data. As mentioned before, device usage in the future will be tied to EHR records and anonymously shared/aggregated to get better metrics on the real patient value provided by the medical equipment.
This is a part of the FDA's UDI roadmap and something to watch in the coming years as hospitals put a premium on value-based care. Imagine knowing what device is best for any given situation, which devices have the most recorded adverse events or what devices led to the most favorable outcomes.
This is the future, and it is attainable.
Information Technology is another stakeholder to consider when understanding the value of reliable data. Information Technology cannot manage security and network capacity without having a valid clean inventory of medical equipment that is on their network.
Last but not least, the Biomedical Engineering team can use clean and reliable medical equipment data to benchmark their cost-of-service ratios against industry standards and analyze data on specific models to optimize maintenance procedures.

Medical equipment is critical to healthcare. Reliable medical equipment data is not just for scheduling preventative maintenance and fixing failures. Making this data accessible to other hospital administrators is foundational to improving healthcare outcomes. Starting with a focus on reliable and accessible data will ensure that your organization is ready to mature and complete in the new value-based care paradigm.
I have often heard the mantra that “your Biomed Program is only as good as the data in your CMMS.” However, this is only a small part of the bigger picture of how medical equipment data can be used. Your Supply Chain, Finance, clinicians, IT, and value-based programs are also only as good as the available insights about medical equipment. This link is rarely discussed, and I am excited to be working on foundation aspects to enable better healthcare outcomes.
How do you get started? The best place to start is by measuring the reliability of your medical equipment data. Contact us at accruentdatainsights@accruent.com and ask for a free data cleaning report card from Accruent.

Want to lower your medical equipment total cost of ownership (TCO) while improving quality of care? These actionable strategies can help.
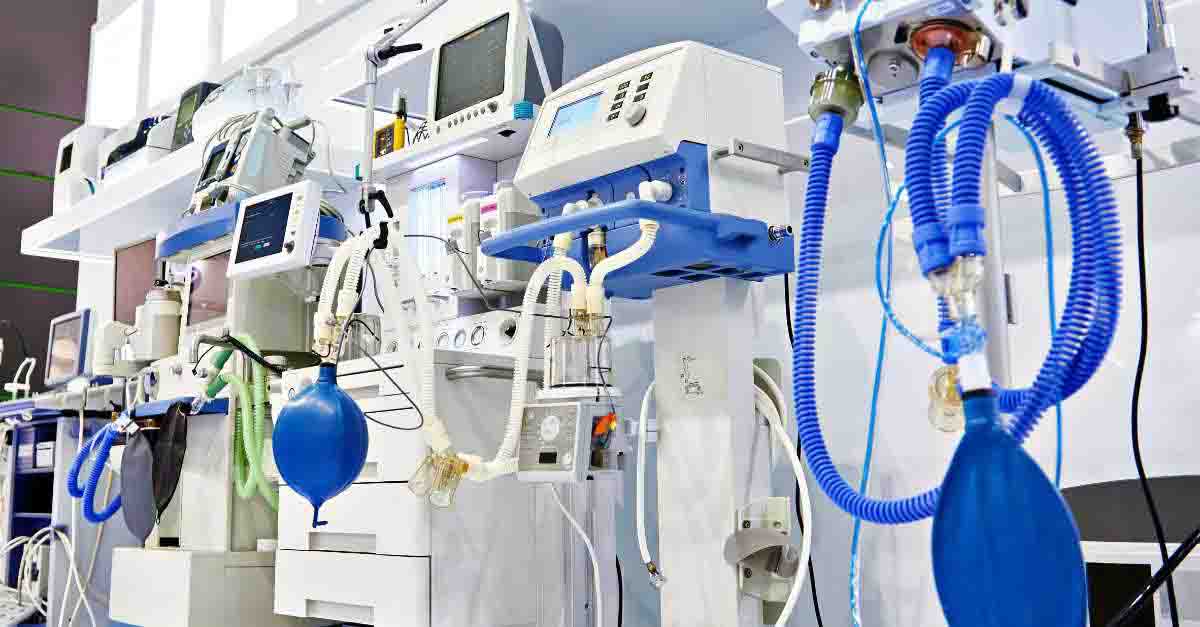
See how standardized medical device manufacturer and model names can help your healthcare HTM department keep your equipment data clean.
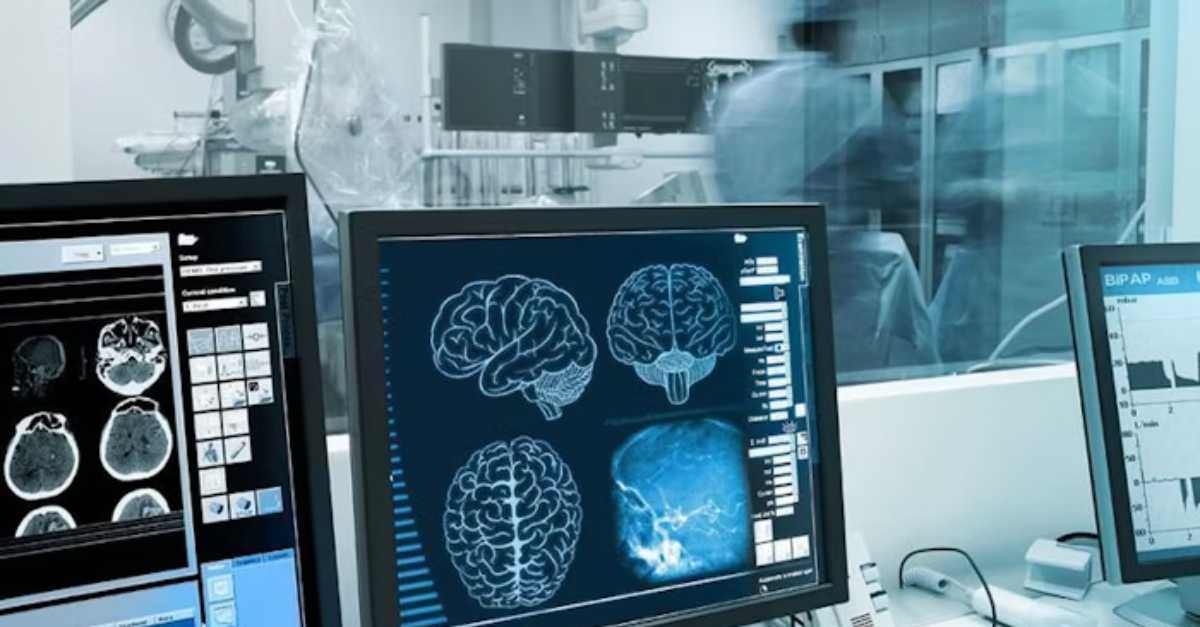
Medical equipment is expensive and extremely important—which means that you don't want to see it lost or thrown away. RFID tagging and other tools ...
Subscribe to stay up to date with our latest news, resources and best practices.
* To unsubscribe at any time, please use the “Unsubscribe” link included in the footer of our emails.