
Mitigating Medical Equipment Cybersecurity Risks with a Modern Healthcare CMMS
Learn the true cost of healthcare cybersecurity, the risks hospitals face, and how to implement an effective cybersecurity strategy.
Solutions
Workplace Management Solutions
Real Estate Management Solutions
Maintenance Management Solutions
Energy Management Solutions
Engineering Document Management Solutions
Asset Management Solutions
Automate campus scheduling for classes, meetings, and exams with our EMS software.
Plan and manage conferences effortlessly with EMS software to impress guests and streamline operations.
Boost workplace flexibility and maximize space use with seamless desk and room booking.
Organize workplace or campus events smoothly, creating memorable experiences.
Optimize workspace, manage allocations efficiently, and reduce costs with our space management solutions.
Deliver projects on time and within budget by improving communication, collaboration, and efficiency with our software.
Streamline lease accounting for ASC 842, IFRS, and GASB compliance.
Manage leases efficiently by tracking key dates, analyzing costs, and ensuring compliance.
Centralize data and analytics for better insights, faster negotiations, and revenue growth.
Centralize facility and asset maintenance, automate work orders, and ensure compliance with our CMMS software.
Extend asset life, reduce downtime, and prevent costly repairs with data-driven monitoring.
Prevent equipment failures and extend asset life by detecting and addressing issues early.
Make sustainable, cost-efficient energy decisions by monitoring and optimizing power consumption.
Remotely monitor and control equipment with real-time data to predict issues, boost efficiency, and reduce downtime.
Easily share and collaborate on documents, creating a single source of truth for engineers and contractors.
Manage and analyze assets across their lifecycle to schedule maintenance, reduce downtime, and extend lifespan.
Improve visibility, automate work orders, and ensure compliance for efficient facility and asset management.
Resources
Browse our full library of resources all in one place, including webinars, whitepapers, podcast episodes, and more.
Self-Service & Support
Looking for self‑service training, best practices, helpful videos, product resources, or support? You’re in the right place.
About Accruent
Get the latest information on Accruent, our solutions, events, and the company at large.
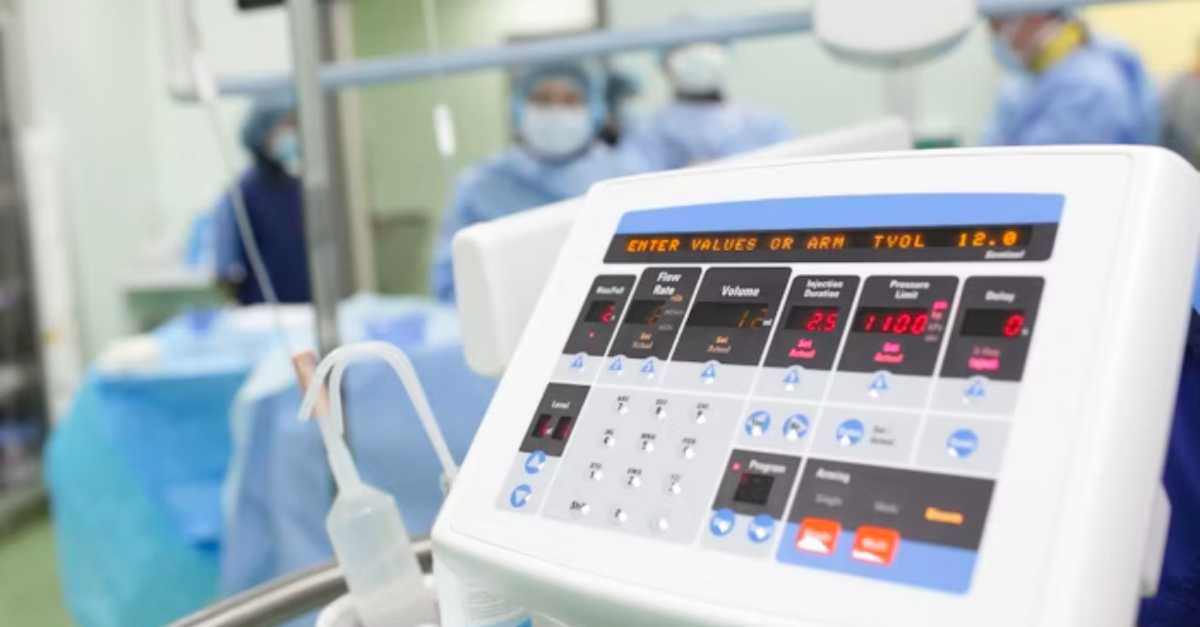
Discover many common challenges facing hospital departments, how to streamline operations, and what to look for in a CMMS solution.
Most hospital healthcare technology management (HTM) departments today use a Healthcare Computerized Maintenance Management System (CMMS) to reduce asset downtime and organize maintenance workflows. However, many are legacy CMMS solutions that only provide work order management and do not integrate with other systems throughout the organization or provide the technological innovation needed to keep up with the advances in healthcare asset management.
The asset and maintenance management industry stands on the edge of several fundamental shifts that will shape the future of the industry. Healthcare systems are struggling to keep pace with the digital transformation taking place, and HTM departments risk being outsourced if they do not find ways to automate and connect their systems.
Legacy CMMS solutions are not designed to manage today’s highly specialized biomedical devices and machines, optimize supply chain issues, assess the rising tide of cybersecurity threats that continue to bombard the healthcare industry or address the regulatory concerns that come with more complex assets.
A truly modern healthcare technology management CMMS software solution can transform your HTM department, enhance the patient experience, mitigate costly cybersecurity risks, reduce operating costs, enhance operational efficiency within the institution, and provide ongoing compliance with policies, laws and regulations.
To keep up with the times, HTM departments need to modernize their CMMS to keep up with the rapid technological advancements in healthcare. It is also critical that the CMMS be able to manage cybersecurity initiatives, Alternative Equipment Maintenance (AEM) programs, equipment capital planning and the complete asset lifecycle—and go far beyond simple work order management.
Meanwhile, the COVID-19 pandemic continues to take a toll on America’s healthcare infrastructure and operating margins, and there are growing concerns about cybersecurity risks, the effects of the aging workforce and regulatory compliance.
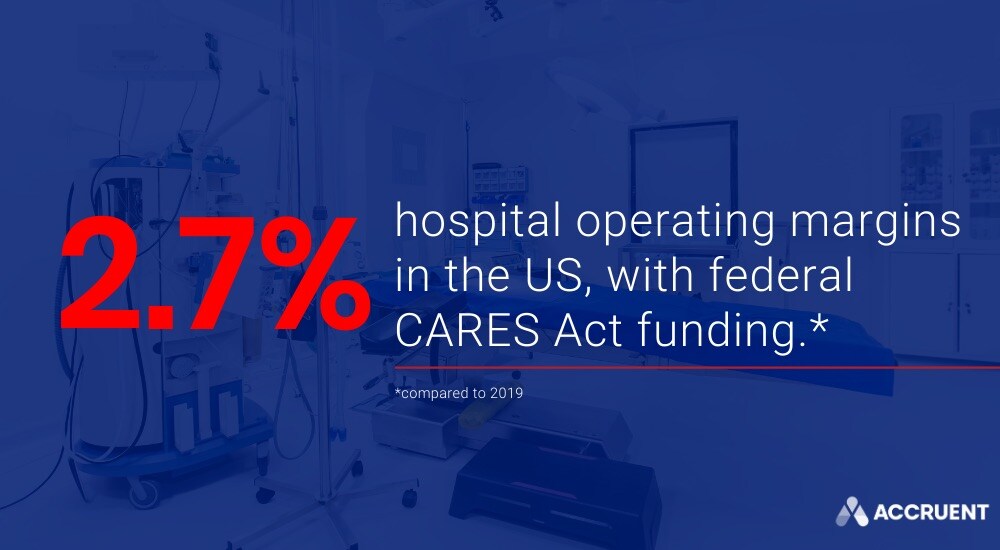
The COVID-19 pandemic continues to create a difficult, uncertain operating environment for the nation's hospitals and health systems, according to Kaufman Hall’s October 2020 National Hospital Flash Report. Hospital operating margins are well below 2019 performance at 2.7% through September with federal Coronavirus Aid, Relief, and Economic Security (CARES) Act funding, and -1.9% without CARES funding compared with the first nine months of 2019.
Hospitals and clinics all over the country are facing the problem of an aging biomedical technician workforce. There soon will not be enough technicians to maintain and service their growing pool of critical biomedical equipment, and there are not enough young people entering the field. The mean age of radiology technicians has risen from 50 to 52.4; the age of level-three biomed technicians has risen from 49 to 52; and overall, the age of healthcare technicians has risen from 49 to 51.
Hospital biomedical and clinical engineering departments continue to be asked to do more with less, while also dealing with a workforce shortage. Implementing a well-designed alternative equipment maintenance (AEM) program can reduce an HTM department’s preventive maintenance (PM) time while maintaining equipment safety and regulatory compliance.
For any potential AEM decision that is to be made, an extensive amount of data is needed to support it. Not only must you have a good rationale for making deviations for procedures or intervals, you also must be able to perform continuous monitoring of failure rates to ensure these deviations have not negatively impacted safety. Legacy CMMS solutions do not provide the data needed to develop a compliant AEM program.
These days, almost all biomedical devices used in hospitals have embedded, network-connected technologies. Medical devices such as monitors, infusion pumps, ventilators, CT and MRI scanners all have critical patient information that could be accessed or tampered with. Single points of failure could open the door for hackers to take out significant portions of a hospital's medical network and affect patient safety.
Cyber-attacks are only expected to get worse. In October 2020, U.S. government agencies warned hospitals to brace for an increased and imminent wave of ransomware cyberattacks that could compromise patient care and expose personal information and urged providers to step up their defenses.
Recent attacks in October 2020 on hospitals in California, New York and Oregon are believed to be part of the massive Ryuk ransomware attack, which comes just weeks after the same malware attack hit a U.S. system with 250 care sites. That attack forced computer systems offline and encrypted hospital services, causing ambulances and surgical patients to be redirected in the aftermath.
One of the most important responsibilities of an HTM department is to ensure the hospital is compliant with all laws and regulations impacting its biomedical devices. Compliance standards require a 100% completion rate for scheduled maintenance activities of every medical device—whether the device is “high risk” or “non-high risk”—but they do not specify how to implement the standards. This creates a challenge for hospitals.
HTM organizations use their computerized maintenance management system (CMMS) as the primary tool to document regulatory compliance. However, what the HTM industry has discovered is that CMS, the Joint Commission, and other regulatory bodies change their standards often and legacy CMMS are not able to keep up with the changes.
Although progress is being made to prevent healthcare-associated infections (HAI), the Center for Disease Control (CDC) estimates one in 31 hospital patients acquires at least one HAI. Hospitals must consider how they can improve hospital equipment maintenance management to reduce infection risks.
Your healthcare system can mitigate infection risk by properly scheduling and maintaining biomedical equipment, improving equipment utilization and staff request fulfillment times and applying consistent medical equipment cleaning and disinfecting processes.
Now more than ever, the right supply chain strategies are needed to increase your hospital’s equipment availability and utilization rates to free up scarce resources and alleviate shortages. When equipment is not available for clinical staff, it creates perceived shortages, friction between departments and hinders a hospital’s ability to find equipment for preventive maintenance and recalls, putting patient safety at risk and creating a liability hazard.
Two ways healthcare organizations typically address the perceived medical equipment shortage issues is purchasing additional new equipment or renting equipment. In fact, many hospitals typically stock more equipment than they need. This is particularly true with mobile medical equipment like IV Pumps, Sequential Compression Devices (SCDs), Feeding Pumps, and PCA pumps. But the bigger problem is that existing equipment is only being used at a fraction of its potential.
For example, the average utilization rate for an IV pump is 40%. With improved strategies using a modern healthcare CMMS, that rate can be improved to at least 60%, and to more than 75% in optimal cases. This practice can eliminate most of your rental costs and help you potentially avoid over a million dollars in capital purchase expenses.
HTM departments have long provided key post-acquisition support and management of medical equipment with planned and corrective maintenance throughout their useful life. While these are extremely important functions, there are some significant missed opportunities if departments are not involved in all phases of asset management—from pre-planning of assets to the point of their final disposition. Being an integral part of the capital evaluation, assessment and receiving processes on the front end and reallocation and disposal on the back end brings additional value to your organization.
Legacy CMMS solutions limit the ability to obtain meaningful operational data needed for optimized full-life cycle medical device management, which costs healthcare systems time, effort and financial resources.
In addition to these challenges, healthcare systems often face:
Healthcare systems are employing a variety of strategies to combat shrinking margins and rising costs. Many hospitals and health systems have reduced costs and efficiencies at the margins of their organizations, but long-term sustainability may require a fundamental, digital transformation of the way that services are organized and delivered. A modern healthcare CMMS can help.

Healthcare facilities have a lot of medical equipment and confidential data that needs to be managed efficiently. Any inefficiency in managing biomedical equipment can not only affect employee productivity but also increase the liability risk. This calls for a modern computerized maintenance management system that goes beyond documentation and work order management.
A modern healthcare CMMS software solution streamlines biomedical asset maintenance management functions and will:
A CMMS that was great to start with may not have the ability to hold up over time or through any major business changes, especially digital transformation of a healthcare system. Keeping a diligent eye out for the signs of a limited system will make it apparent when you need to replace your maintenance solution.
Although reasons to replace a legacy CMMS for a modern healthcare CMMS are usually straightforward, it is not always apparent that your maintenance solution is falling behind, and any loss of forward progress can set your maintenance ROI on an unexpected downturn.
Here are signs that will let you know it is time to replace your maintenance solution:
In today’s healthcare business environment, electronic record keeping is the norm. Patient records, appointment bookings, visibility of upcoming events, personnel records, procurement activities and even food management for patients are all submitted, fulfilled and retained electronically.
Going digital and analyzing digital records allows HTM organizations to consume benchmarking data at many levels and to:
A modern healthcare CMMS and digital records benefit a healthcare system with efficiency gains, accuracy gains, accountability gains, consumption gains, as well as the ability to benchmark data.
The ability to determine the average turn-around time for specific job types can allow HTM departments to schedule repair activities instead of always being reactive. Accessing digital records of past maintenance activities and combining that data with a forecast of future scheduled activities also allows an HTM department to provide definitive data to create a successful AEM program and to forecast budget and manpower needs.
The Internet of Things (IoT) is the interconnection of computing devices embedded in everyday objects that enables them to send and receive data. Alongside the invention and adoption of IoT, the evolution of sensors has reached a new level and is becoming an industry standard. These sensors placed on your critical assets, with the help of thresholds set in a modern healthcare CMMS, can help to predict failures and avoid downtime. Reactive maintenance can cost a company up to eight times what establishing a preventive maintenance program can save in reducing downtime.
Sensors placed on medical devices allow for automated data collection, providing insight into the equipment’s location and condition. Each asset and device in the hospital typically has unique technical requirements for connecting to the cloud and a computerized maintenance management system. Challenges with locating assets can be resolved by using Active RTLS (real-time locating systems) or Passive RFID (radio-frequency identification), while equipment condition challenges can be resolved by monitoring temperature, humidity and utilization in real time.
Monitoring the storage temperature of critical assets and supplies across hospital and pharmaceutical environments is required to ensure safety and compliance. RTLS temperature monitoring is a proactive measure by healthcare providers to ensure the integrity of items such as blood, food, medications, and tissue samples. Actively monitoring the critical temperatures of these items helps hospitals eliminate manual regulatory documentation and paper log reporting and save thousands of dollars a year in loss prevention due to incorrect storage temperatures.
For the healthcare industry, there’s an opportunity to preserve often expensive or even irreplaceable products such as pharmaceuticals, vaccines, or human organs and tissues that must be stored at a constant temperature. Efficient maintenance of cold storage units enabled by a revolutionary, yet straightforward IoT solution provides enhanced patient care and improves the bottom line.
Medical device networks require consolidation of biomedical and IT departments to effectively leverage digital tools and provide better network security. The rising dependence on smarter, more complex and costlier assets in a digital age means that these assets’ failure can bring catastrophic consequences.
An integrated HTM department can make a dramatic, positive improvement to any healthcare organization through reduced costs, higher accuracy, faster response, better healthcare asset management and increased customer service.
Managing the full asset lifecycle—from pre-assessment through acquisition and support to final disposition—is the only way to truly know and reduce the total cost of ownership for your medical assets.
Transformative CMMS and Asset Management designed exclusively for healthcare enables organizations to:
If you have a legacy maintenance solution, you probably already track the warranties, inspections, routine maintenance and repair history of your equipment. However, if keeping up with compliance codes and industry regulations is more of a manual process, you may want to consider replacing your maintenance solution.
A modern Healthcare CMMS can automate compliance tasks by setting notifications, scheduling routine maintenance, tracking a repair history log and organizing important documents (e.g., equipment manuals, spec sheets, ID tags) for each of your assets. This not only saves clinical engineers time and can boost compliance rates, it will also make inspections and audits a breeze since everything is documented and easily accessible.
Since HTM departments must comply with hundreds of regulations, it is critical to have a CMMS/EAM that can identify, document, record and report on all medical devices to maintain efficient and compliant operations.

Growing competition and slashed budgets require that hospitals work at maximum efficiency to stay competitive and compliant. Investing in a modern CMMS is the easiest way for healthcare organizations to streamline operational efficiency and increase profits while staying complaint with constantly changing policies, laws and regulations and mitigating cybersecurity risks.
For clinical engineers who value precise data to track asset health and to automate services and equipment distribution requests, and IT departments who need detailed information and predictive analytics to ward off medical device cyber-attacks, a suite of connected tools, sensors and databases in a modern healthcare CMMS can be as essential as traditional tools and test equipment.
The best healthcare CMMS software solutions are mobile-enabled and web-based CMMS solutions that manage all aspects of asset management (medical devices, facility equipment and biomedical equipment), work order management, financials and expenses, preventive maintenance, risk and compliance reporting, equipment distribution and more. A modern healthcare CMMS provides:
Healthcare organizations that leverage advanced CMMS and Asset Management technology can increase utilization rates and breakdown operational silos. In addition, systems that employ these solutions to lower associated costs, increase equipment availability, and offer patients, visitors and staff a better experience and greater peace of mind.
Beyond technology, Accruent experts are available to evaluate your current processes, key performance indicators and highlight step-by-step improvement recommendations to make your Healthcare Technology and Biomedical Departments a Strategic Asset.
Contact us today to start a conversation about how Accruent can transform your asset management strategy.

Learn the true cost of healthcare cybersecurity, the risks hospitals face, and how to implement an effective cybersecurity strategy.

If you're using an outdated healthcare CMMS, you could be costing your business more than you know. Here's why having the right tech matters.
Learn about how smarter healthcare systems can help you save money and provide industry-leading patient care.
Subscribe to stay up to date with our latest news, resources and best practices.
* To unsubscribe at any time, please use the “Unsubscribe” link included in the footer of our emails.